Back Pain and Depression
Healthcare professionals have been aware for a long time that people suffering with chronic pain especially of the back, are at a higher risk of developing depression. Research has also now shown that those suffering depression are also more at risk of developing a chronic pain condition. This starts a cycle of events that can spiral without treatment.
It is very common for sufferers of chronic back pain to develop depression, and it is the most frequently associated mental condition with the incidence of chronic back pain.
Signs and Symptoms
The symptoms of depression are inter-linked with those of back pain. Back pain can lead to a disturbed sleeping pattern meaning that mood can be negative during the day, along with fatigue. A lack of sleep and muscle fatigue increases the risk of injury.Back pain can cause a reduction in mobility, so everyday activities and employment can be affected, leading to social isolation; depression is made worse by withdrawing from normal society and black moods can increase in frequency and duration.
Other symptoms that can appear with both conditions are feelings of being blue, lonely and a change in appetite. A reduction in nutrients will slow the recovery or healing process on the back injury.
Effects of Back Pain and Depression
Chronic back pain can affect an individual’s ability to work, this can lead to money worries which can cause or exacerbate symptoms of depression.Sexual ability and function may be altered with the incidence of back pain; this could cause tension in relationships, as can a reduction in the participation in everyday family activities.
Research has shown a link between delayed healing after surgery in those who are suffering with depression. It is recommended that the depression is treated prior to surgery where possible. There is also valuable research that has shown a link between the incidence of depression and the likelihood of a back pain recurrence.
Treatments
Sufferers of chronic back pain should be treated for the underlying cause of the pain if it can be found, with the doctor performing an evaluation of mental state at the same time.Doctors are very aware of the analgesic effects of prescribing an anti-depressant medication for its pain relieving properties; in fact on occasion an anti-depressant will be prescribed for its analgesic benefits alone, even without the patient having any symptoms of depression.
The most common anti-depressant used for its pain relieving qualities is called Amitriptyline.It has been found that anti-depressant medication can be useful in the treatment of fibromyalgia, rheumatoid arthritis, osteoarthritis and cancer pain.
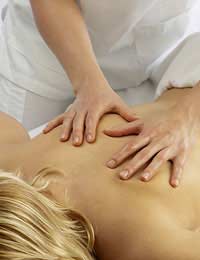
Other treatments that can help treat both chronic back pain and depression together can include massage, hypnotherapy and gentle exercise. Massage can help relieve stress, therefore lowering a risk factor of developing depression and also helping relieve the tension in muscles that can add to pain levels. Hypnotherapy can help the individual gain some control over their feelings and pain levels and may increase concentration and memory, both of which may be affected by depression and chronic pain. Exercise allows for social interaction and as a method of relieving pain. Sunshine and fresh air may also contribute to lifting the person’s mood.
Tasks should be broken down into more manageable jobs and should be completed in a realistic time frame; this allows for maintaining independence and helps with mobility issues.
Anyone who is feeling depressed should be aware of its link with the development of chronic pain conditions and sufferers of long-term back pain should be aware of the risks of suffering from depression.
Your GP will help you make decisions that are beneficial to you; this may include counselling to help with the management of pain in everyday life and to help cope with living with depression.
- Back Pain and Shingles
- Back Pain and Evolution
- Healthy Eating and Back Pain
- Back Pain and Hernia
- Ageing, Losing Height and Back Pain
- Bad Back: A Sign of Too Much Surfing?
- Back Pain and Athletes
- What is Spinal Muscular Atrophy?
- How is Psoriasis Linked to Back Pain?
- Back Pain Nearly Ruined My Pregnancy: A Case Study
- Back Pain and Parkinson's Disease
- Facet Syndrome or Facet Joint Disease
- Bags, Backpacks and Back Pain
- Can Back Pain Be all in the Mind?
- Infection and Back Pain
- Can Shoes Cause Back Pain?
- Back Pain and Cancer
- Smoking and Back Pain
- Weight Gain and Back Pain
- Osteoporosis and Back Pain
- Causes of Back Pain: Herniated Intervertebral Disc
- What is Lumbar Spinal Stenosis?
- How Does Your Bed Affect Your Back?
- Coccydinia
- Cauda Equina Syndrome
- What Is Fibromyalgia And How To Deal With It
- Dehydrated Discs
- Office Chairs And Back Pain
- Slipped Disc
- Tilted Pelvis
- Spinal Stenosis Explained
- What is Sciatica?
- Back Pain and Pregnancy
- Spinal Fractures
- Strains, Sprains and Back Pain
- Injuries and Trauma and Back Pain
- Spinal Dislocation
- Ligament Damage and Back Pain
- Sudden Movements and Back Pain
- Who is at Risk of Developmental Back Pain?

Re: Who is at Risk of Developmental Back Pain?
I have been getting muscle spasms in my lower back for 30 years and when they occur I walk like an old man. I…
Re: A Spinal Tap Caused My Back Pain
When I was 14 I was sent to the emergency room with an illness the doctors couldn't identify. Extremely high fever and high…
Re: A Spinal Tap Caused My Back Pain
I've had spinal meningitis 7 times now. So much scar tissue they have to do x ray with the lumbar puncture. I am having a lot…
Re: A Spinal Tap Caused My Back Pain
Hello I had spinal tap done bout 8 month ago due to a brain aneurysm. I tell you someday they way my back is make me not…
Re: A Spinal Tap Caused My Back Pain
So about 7 or 8 months ago I got a spiral tap preformed due to have being diagnosed with Idiopathic intracranial…
Re: A Spinal Tap Caused My Back Pain
So about 7 or 8 months ago I got a spiral tap preformed due to have being diagnosed with Idiopathic intracranial…
Re: Dehydrated Discs
hI THERE, I have Dyhydration L3/l4 and ll4/l5 and disprotrusion and sequestrated discu after MRI i am aged 52. I had hip pain all night for 3…
Re: A Spinal Tap Caused My Back Pain
Hi . I also had a spinal Tap to check the stages of a bleeiding in my brain. This has caused me serious back pain almost…
Re: Dehydrated Discs
Alex - Your Question:I am a 27 yr old male who up until last year was working 84-108 hrs/week and always had back problems but all the doctors I…
Re: Dehydrated Discs
I am a 27 yr old male who up until last year was working 84-108 hrs/week and always had back problems but all the doctors i had seen told me its…